Getting Relief from Sciatica - Causes, Symptoms, and Treatments
Posted on 01-11-2023 01:51 PM

Sciatica is a condition characterized by pain that radiates along the path of the sciatic nerve, which branches from the lower back down through the hips and buttocks and into each leg.
It is a common condition, with estimates of lifetime incidence ranging from 10-40% of the population. While sciatica can be quite painful and debilitating, the good news is that the vast majority of cases resolve on their own with time and conservative treatment, without the need for surgery.
However, seeking early diagnosis and treatment is key to finding relief as quickly as possible and preventing ongoing problems.
What Causes Sciatica?
The sciatic nerve is the largest and longest nerve in the body, starting in the lower back and extending through the buttock and down the leg to the foot.
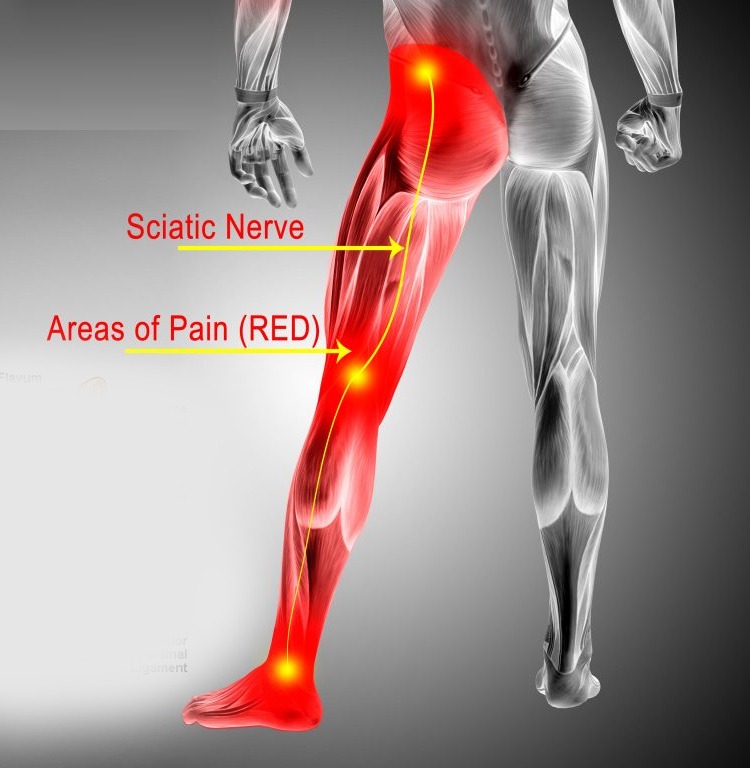
Sciatica occurs when this nerve becomes irritated, inflamed, or compressed, resulting in pain that radiates out from the lower back and through the path of the sciatic nerve.
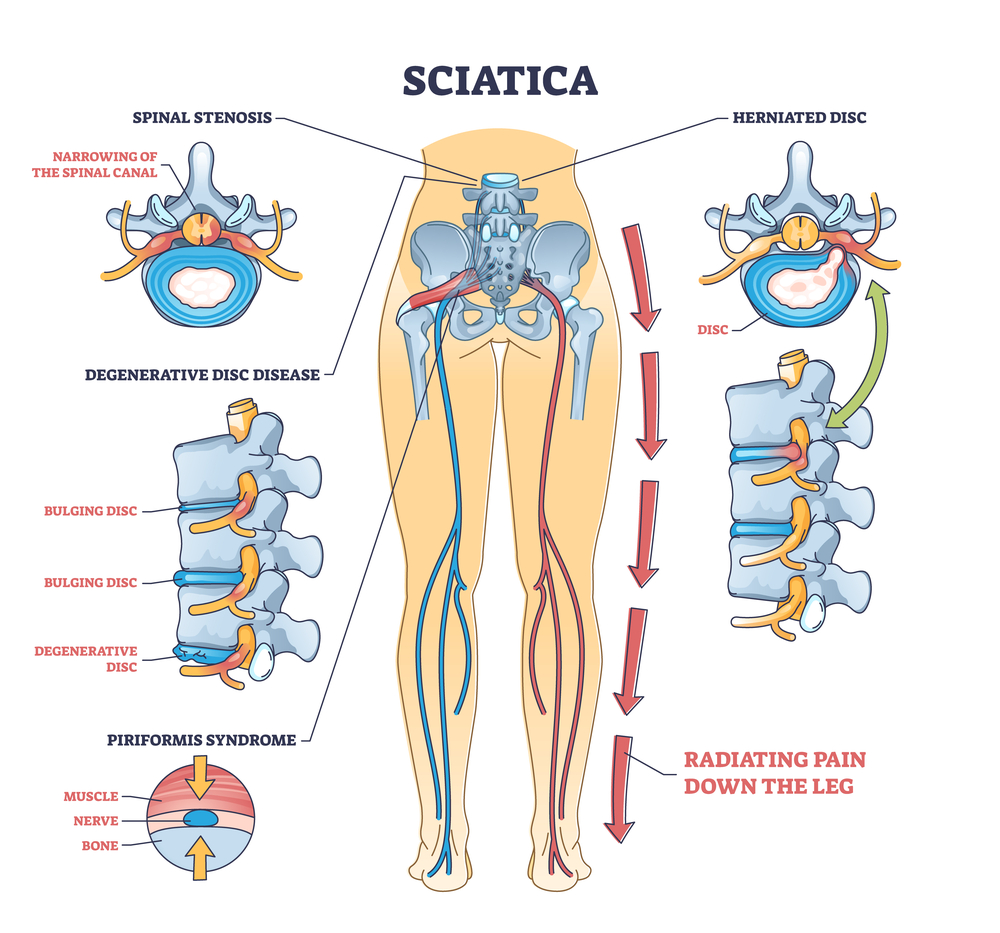
There are several potential causes of sciatic nerve irritation:
- Herniated discs - Discs are gel-filled cushions between the vertebrae that can bulge or rupture, putting pressure on the adjacent sciatic nerve. This is one of the most common causes of sciatica.
- Bone spurs - Bony growths called bone spurs can develop on the spine and irritate or compress the sciatic nerve. Spinal stenosis, or narrowing of the spinal canal, is often caused by bone spurs or disc bulging.
- Inflammation - Swelling around the sciatic nerve from injury or conditions like pregnancy or infection can trigger sciatica.
- Piriformis syndrome - The piriformis muscle runs very close to the sciatic nerve. If this muscle spasms or tightens, it can pinch the sciatic nerve and result in sciatic pain.
The Sciatic Nerve: Anatomy and Function
The sciatic nerve is the largest and longest nerve in the human body. It starts in the lower back and extends through the hips and buttocks down the back of each leg to the feet.
Anatomy
The sciatic nerve is formed from the nerve roots exiting the lumbar spine at L4, L5, S1, S2, and S3. These roots combine to form a thick nerve bundle that passes through the pelvis. After emerging from the pelvis through the greater sciatic foramen, the unified nerve runs under the gluteus maximus muscle and descends down the back of the thigh. It branches below the knee into the tibial nerve and common fibular nerve, which provide innervation to the lower leg and foot.
Function
- Motor function - The sciatic nerve innervates the muscles of the hamstrings in the back of the thigh as well as most of the muscles below the knee that allow for foot and toe flexion and extension. It provides the motor signals needed for bending and straightening the leg and moving the ankles and toes.
- Sensory function - The sciatic nerve conducts sensory information from the skin of the foot, calf, thigh, and buttock region on the back of the leg. It carries signals about pain, temperature, and touch to the central nervous system.
- Reflexes - The sciatic nerve contributes to key reflex arcs like the knee-jerk reflex that provide automatic, protective responses to stimuli.
Effects of Damage
Because the sciatic nerve supplies major muscles involved in leg movement, injury or compression can cause:
- Muscle weakness or paralysis in the lower leg and foot
- Numbness or loss of sensation in the back of the thigh, calf, or sole of the foot
- Loss of reflexes like the knee or ankle jerk reflex
- Gait abnormalities like foot drop from inability to lift the foot properly during walking
Sciatica Versus Lumbar Radiculopathy
Sciatica and lumbar radiculopathy both involve nerve compression that leads to radiating leg pain, so they are closely related conditions. However, there are some key differences:
- Cause - Sciatica is a symptom that can be caused by anything irritating the sciatic nerve. Lumbar radiculopathy more specifically refers to compression of spinal nerve roots in the lower back (lumbar spine).
- Location - Sciatica pain radiates down the entire leg, following the path of the sciatic nerve. Radiculopathy pain is often more localized to the lower back, buttocks, and back of the thigh near where the nerve roots are compressed.
- Diagnosis - Sciatica is identified based on symptoms. Radiculopathy involves confirming which spinal nerve roots are affected through imaging or electromyography.
- Treatment - Approaches are similar, but radiculopathy treatment may target specific affected nerve roots through selective nerve root blocks.
Sciatica and radiculopathy are closely linked, but sciatica is the broader, more general term for pain radiating down the leg from any source of sciatic nerve irritation. Radiculopathy pinpoints the cause as compression of specific lumbar nerve roots.
Recognizing Sciatica Symptoms
Symptoms of sciatica include:
- Lower back and leg pain - This is the hallmark of sciatica. Pain often starts in the lower back and radiates down one side through the buttock and down the back or side of the leg.
- Numbness or tingling - In addition to pain, numb or tingling sensations may be felt along the path of the sciatic nerve. This indicates nerve irritation.
- Muscle weakness - Nerve compression can lead to weakness or difficulty moving the leg or foot on the affected side.
- Altered reflexes - The knee jerk reflex may be reduced or absent if the L4 or L5 nerve roots (which comprise the sciatic nerve) are compressed.
The pain from sciatica can range from mild and intermittent to severe and constant. It may be sharp and shock-like or have a burning quality. Often the pain is worse with certain activities like sitting, coughing, or sneezing.
Who Gets Sciatica?
There are a number of risk factors that increase susceptibility to sciatica:
- Age - Degenerative changes in the spine become more common with age, increasing the risk of conditions like spinal stenosis. Sciatica is most common in adults over age 50.
- Obesity - Excess weight places strain on the lower back and can contribute to spinal changes leading to sciatica.
- Occupation - Jobs that involve heavy lifting, twisting motions, driving, or prolonged sitting put strain on the lower back and may predispose individuals to sciatica.
- Genetics - Sciatica can have a hereditary component, especially when linked to causes like spinal stenosis.
- Smoking - Smoking reduces blood flow, leading to disk degeneration, and coughing can increase pressure on the spinal nerves.
- Diabetes - High blood sugar levels associated with diabetes can damage the sciatic nerve over time.
Getting a Diagnosis
If you have symptoms of sciatica, especially moderate to severe pain lasting more than a week or two, it is important to see a doctor for an evaluation. They will take a full medical history and perform a physical exam, which may include:
- Assessing range of motion in the lower back
- Testing reflexes at the knee and in the foot
- Checking for muscle weakness or numbness in the leg
- Having you walk on your toes and heels to observe gait
Your doctor may order imaging tests, such as an X-ray or MRI scan, to get a look at the state of your spine and identify any anatomical causes of nerve compression.
However, imaging is not always needed for a diagnosis if the history and physical exam are conclusive.

Sciatica Treatment Options
There are a variety of treatment options available for sciatica patients, ranging from self-care remedies and physical therapy to medications and injections. Surgery may be considered for more severe cases that do not respond to conservative treatment. The right approach depends on the severity of symptoms and the suspected cause.
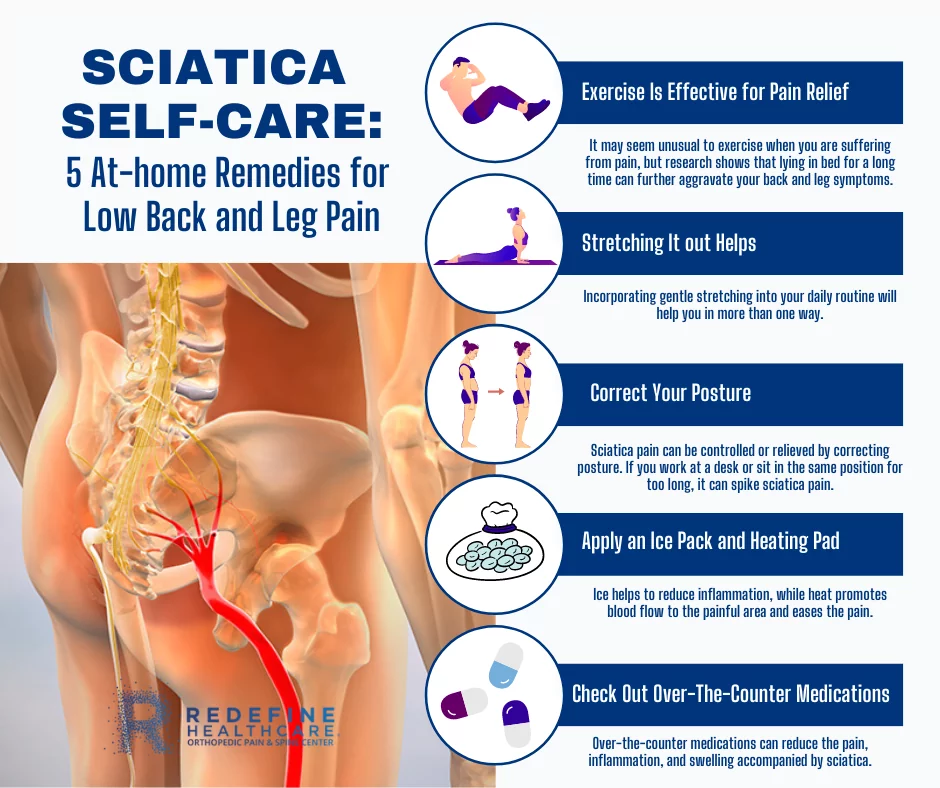
Self-Care Remedies
Milder cases of sciatica often resolve with time and self-care:
- Rest - Take a break from aggravating activities for a day or two to allow symptoms to calm down. But avoid prolonged bed rest, which can make pain worse.
- Cold/heat therapy - Use ice packs or heating pads to the painful areas for 15-20 minutes at a time to reduce inflammation and muscle tension.
- OTC medication - Anti-inflammatory drugs like ibuprofen can relieve pain and swelling.
- Gentle stretches - Light stretching can help reduce muscle tension without straining the sciatic nerve.
- Modify activities - Avoid motions that trigger symptoms, but stay as active as possible within pain limits.
Physiotherapy
Once the initial pain begins to subside, physiotherapy is often prescribed. A physiotherapist can provide sciatica treatments and exercises to help strengthen the core and improve flexibility, reducing pressure on the sciatic nerve.
They may use therapies like ultrasound or muscle stimulation as well. Regular PT is often a key part of recovery.
Medications
If self-care is inadequate for managing sciatic pain, doctors may prescribe stronger medication. These may include:
- Muscle relaxers like cyclobenzaprine
- Oral steroids such as prednisone to reduce inflammation
- Anti-seizure drugs like gabapentin to block nerve pain
- Narcotics for short-term severe pain relief
When sciatica is diagnosed, doctors typically first recommend trying conservative treatments for several weeks to see if symptoms can be managed without surgery.
OTC Medications
Anti-inflammatory drugs like ibuprofen (Advil, Motrin) or naproxen (Aleve) can help relieve pain and inflammation associated with sciatica. Acetaminophen (Tylenol) may also ease discomfort. Check with your doctor about dosage and length of use.
Prescription Medications
If OTC meds are inadequate, muscle relaxants like cyclobenzaprine or narcotics like tramadol may be prescribed for short-term pain relief. Antidepressants and anticonvulsants can also treat neuropathic sciatic pain.
Exercise
Gentle stretches and core exercises like planks and bridges strengthen the back and improve flexibility. However, too-intense activity could worsen symptoms, so discuss exercise regimens with your physician or physical therapist.
Heat and Ice Therapy
Alternating hot and cold treatments can relax muscles and reduce inflammation. Use heating pads or cold packs for 20 minutes at a time, allowing the skin to normalize between applications.
Massage
Deep tissue massage techniques applied to the lower back muscles can help minimize spasms and tension. A certified massage therapist can provide relief without directly manipulating the sciatic nerve.
Spinal Manipulation
Gentle spinal manipulations can improve alignment of vertebrae, taking pressure off compressed nerves. The risks and unknown long-term benefits of manipulation must be carefully weighed.
Acupuncture
Fine needles are inserted in trigger points along the sciatic nerve pathway to relieve blockages in energy flow or qi. Acupuncture has shown some promise for alleviating chronic back and nerve pain.
Interventional Treatments for Sciatica
If conservative treatments do not provide sufficient pain relief after several weeks to months, more invasive interventions may be considered.
Epidural Steroid Injections
Corticosteroid medication is injected into the epidural space around the spinal cord and nerve roots to reduce local inflammation. Pain relief can last for several months, but benefits are often temporary.
Selective Nerve Root Blocks
Anesthetic and steroid medication is injected directly alongside an affected nerve root to numb sensation from that individual spinal nerve. Used diagnostically and therapeutically.
Radiofrequency Ablation
The tip of a needle heats up to destroy nerve fibers carrying pain signals from an irritated nerve root. This can provide sciatic pain relief for 6 months up to 2 years.
Discectomy
Surgical removal of a portion of a ruptured disc compressing the sciatic nerve. This is the most common surgery for symptomatic herniated discs unresponsive to conservative treatment.
Laminectomy
Surgical bone removal to enlarge the spinal canal, decompressing pinched nerves. This can treat spinal stenosis causing chronic sciatica.
Risks and Limitations
Interventions like epidural injections come with risks like bleeding, infection, nerve injury, and lack of pain relief. Surgeries have more serious risks including permanent neurological damage. Conservative treatments should be exhausted first.
8 Exercises to Relieve Sciatica Pain
While rest is important initially, light exercise can actually help reduce sciatic pain and speed recovery. Exercise strengthens the core muscles supporting the lower back and improves flexibility, taking pressure off the sciatic nerve. Here are 8 easy exercises to try:
1. Knee to Chest
- Lie on back, bring one knee up to chest, grasp hands behind thigh
- Hold for 20 seconds, relax, repeat on opposite side
- Stretches lower back
2. Lumbar Rotation
- Lie on back with knees bent, drop bent legs to one side
- Keep shoulders on floor, hold for 30 seconds
- Repeat to other side, stretches lower back muscles
3. Bridge
- Lie on back, bend knees, lift hips up off floor
- Hold for 30 seconds, relax, repeat 2-3 times
- Strengthens back, glutes, and hamstrings
4. Child’s Pose
- Kneel on floor, sit back on heels, walk hands forward
- Let torso sink to thighs, hold for 30 seconds
- Stretches lower back, relieves nerve compression
5. Piriformis Stretch
- Lie on back, cross one ankle over opposite knee
- Grasp behind thigh of bent leg, pull toward chest
- Hold for 30 seconds, repeat on other side
6. Hamstring Stretch
- Lie on back, loop strap around foot, straighten leg
- Keep leg on floor, pull strap to stretch hamstring
- Hold for 30 seconds, switch legs
7. Seated Spinal Twist
- Sit on floor, cross right foot over left knee
- Grasp right knee with left hand, twist upper body right
- Hold for 30 seconds, repeat on opposite side
8. Walking
- Walking gently stretches the lower back muscles and stimulates circulation
- Start with short walks and gradually increase distance
Always warm up muscles before stretching with light cardio or calisthenics. Stretch gently within your limits of discomfort. Proper form prevents injury.
When Is Sciatica Surgery Necessary?
Most patients with sciatica improve within weeks to months with conservative treatment and do not require surgery. However, surgery may be considered if:
- Debilitating leg pain persists longer than 4-6 months
- Significant functional impairment prevents normal daily activities
- Progressively worsening leg weakness signals advancing nerve damage
- Cauda equina syndrome with bladder/bowel dysfunction develops
- Large disc herniation on imaging compresses multiple nerve roots
- Spinal instability requires fusion or instrumentation
Common Sciatica Surgeries
- Laminectomy - Removal of lamina bone to decompress nerves
- Discectomy - Partial removal of herniated disc material
- Foraminotomy - Widening of vertebral foramen opening to decompress nerve
- Spinal fusion - Joining vertebrae together for stability
Surgery aims to relieve pressure on the sciatic nerve roots. Outcomes are often good, but benefits must be weighed against risks like infection, blood clots, and anesthesia complications. Surgery is turned to only when clearly clinically warranted.
Sciatica in Pregnancy
Sciatica occurs in up to 45% of pregnancies. While not directly due to pregnancy weight gain, hormonal and anatomical changes during pregnancy increase the risk of developing sciatica.
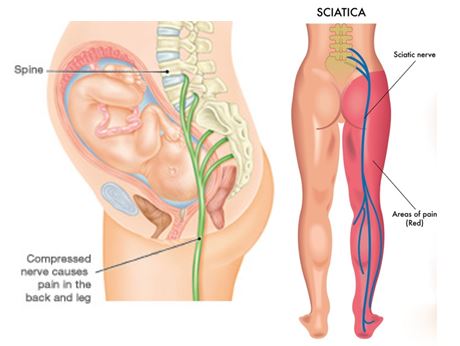
Causes
-
Expansion of the uterus can put pressure on the sciatic nerve.
- Joint laxity from increased estrogen and relaxin hormone levels allows more slippage and misalignment of the pelvic bones and lower spine.
- Fluid retention and swelling (edema) in the nerves can cause irritation.
Symptoms
The classic symptoms of lower back and leg pain may begin during the 2nd or 3rd trimester. Pain, numbness, and weakness usually impact only one side and are often worse when standing or walking.
Treatment
- Gentle stretches, yoga, aerobic exercise
- Hot or cold therapy
- Supportive pillows and braces
- Massage
- Acupuncture
- Pain medication if approved by OB-GYN
Symptoms typically resolve within 3 months after delivery as edema resolves and mobility improves. Seek medical guidance to ensure appropriate pain management during pregnancy.
Sciatica in the Elderly
Sciatica becomes more common as people age. Factors such as spinal degeneration, decreased activity, diabetes, and arthritis make the elderly more susceptible. Diagnosis can be challenging because typical symptoms may be attributed to normal aging.

Age-Related Causes
- Spinal stenosis from arthritis and disc degeneration
- Spondylolisthesis (vertebral slippage)
- Diabetic nerve damage
- Poor muscle strength
- Frailty and falls leading to nerve compression
Warning Signs
Seniors may have vague chronic back, buttock, and leg pain rather than classic sciatica symptoms. Or they may dismiss symptoms as just signs of aging. Sudden trouble walking or standing could indicate a new nerve issue.
Treatment Considerations
Conservative treatment is still preferred, but medicine dosages, exercise regimens, and interventional procedures may need tailoring for older patients. Surgery only as a last resort due to anesthesia risks. Prevent falls, control diabetes, stay active.
Prognosis
Sciatica can take longer to resolve in seniors, but recovery remains likely with proper treatment. Communicating about all symptoms and concerns facilitates the best outcomes for elderly sciatica patients.
When to See a Doctor About Sciatica
Mild sciatica often improves with self-care. But you should make a medical appointment if:
- Pain lasts more than 1 week without improvement
- Symptoms significantly interfere with daily activities
- You have numbness, tingling, or muscle weakness
- You have a history of diabetes, cancer, or back surgery
- Pain extends below the knee or into both legs
- Self-care remedies provide no relief
- You develop any bladder, bowel, or sexual dysfunction
Seek immediate emergency care for:
- Loss of bladder or bowel control
- Sudden severe numbness or muscle weakness
- Fevers, chills, nausea, or vomiting
- Intolerable pain unaffected by medication
- Difficulty walking unaided or foot drop
These red flag symptoms may indicate a serious problem requiring urgent evaluation to prevent permanent nerve damage. Better to err on the side of caution.
6 Tips to Help Prevent Sciatica
Not all cases of sciatica can be prevented, but adopting healthy lifestyle and spine-sparing habits can reduce your risk of developing this painful condition.

1. Exercise regularly
Strength training and low-impact cardioexercise improve core muscle tone. Strong back muscles better support the spine.
2. Maintain proper posture
When sitting and standing, keep the ears, shoulders, and hips aligned. Avoid slouching and hunching over.
3. Use good lifting mechanics
Lift with the legs, keep loads close to the body, avoid twisting motions.
4. Manage weight
Excess weight strains the lower back. Losing even 5-10 lbs can make a difference.
5. Take frequent breaks when driving
Long periods of sitting can irritate back and sciatic issues. Stand, stretch, and change positions.
6. Stop smoking
Smoking impedes disk health. Coughing from smoking also stresses the lower back.
Making back health and strong posture a priority in your daily habits can help keep your sciatic nerve pain-free.
Frequently Asked Questions About Sciatica
What are the first signs of sciatica?
The most common initial symptoms are lower back pain radiating down one leg, sometimes with numbness, tingling, or weakness on the affected side. Pain may be mild at first and worsen over time.
Does sciatica ever affect both legs?
It is possible but uncommon to experience sciatica pain on both sides. This indicates very severe central spinal compression likely requiring urgent medical attention.
Is sciatica a lifelong condition?
For most people, sciatica is an acute condition lasting days to weeks, not a lifelong affliction. Only about 1-2% go on to develop chronic sciatic pain lasting more than a year.
Can you have sciatica without back pain?
It is uncommon, but possible in some cases, to have sciatic nerve pain isolated to the buttock and leg without significant back pain. This can happen with a severe muscle spasm in the piriformis muscle, for example.
How is sciatica diagnosed?
A physician diagnoses sciatica based on the patient’s description of pain radiating down the leg, a physical exam showing neurological changes, and sometimes imaging tests if the cause is uncertain. There are no blood tests or other specialized tests for sciatica.
Conclusion: Finding Relief from Sciatic Nerve Pain
Sciatica is often described as an excruciating condition. If you are experiencing symptoms, the most important thing is to consult a doctor for an accurate diagnosis and appropriate treatment recommendations. While up to 90% of sciatica resolves on its own, getting medical care can help speed your recovery and may allow you to avoid unnecessary complications or suffering. Be sure to call your doctor promptly if you have any sciatic symptoms paired with loss of bowel/bladder function, fever, severe or progressive neurological deficits, or unbearable pain. With today's treatment options, from ergonomic tips to oral medications to epidural steroid injections, most cases of sciatica can be managed effectively without the need for risky surgery. While it may take patience, consistency, and time, relief from sciatic nerve pain is within reach.